Simple Guide to the Endocannabinoid System (ECS)
General info only — not medical advice. Always talk to a qualified prescriber.
The ECS is your body’s balancing network—it helps steady stress, mood, sleep, pain, memory, and inflammation. Medicinal cannabis compounds (like CBD and THC) can interact with this system under doctor-led care.
Research suggests potential benefits such as neuroprotection, anti-inflammatory action, anti-anxiety/antidepressant effects, antipsychotic potential (CBD), and anti-kindling effects for some seizure disorders.

The ECS — The Body’s Inner Regulator
Parts of the ECS
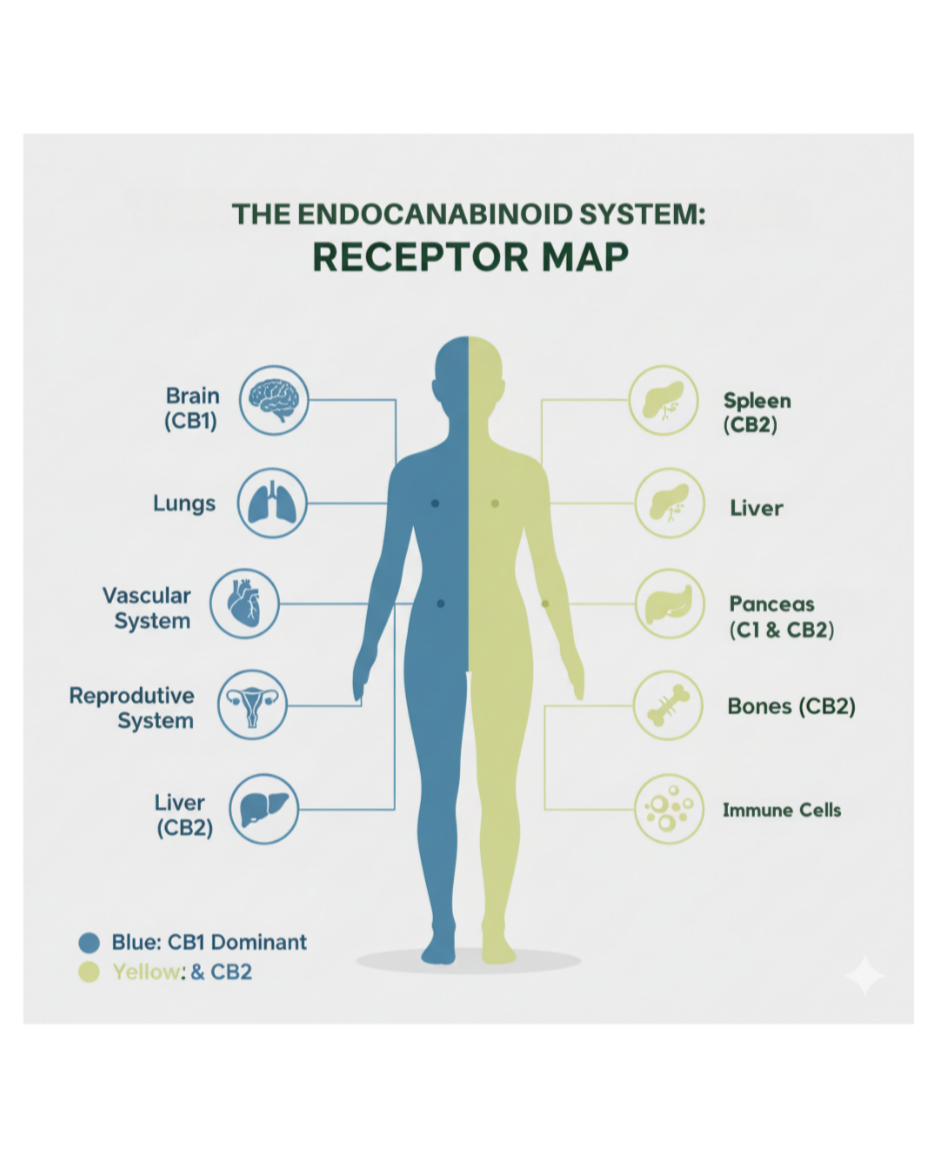
Receptors:
CB1 — mostly in the brain/nerves (memory, sleep, pain, fear learning).
CB2 — on immune cells and throughout the body (inflammation, recovery).
Your own messengers:
Your own messengers:
Anandamide (AEA) and 2-AG — made on demand when you need them.
Enzymes:
FAAH and MAGL — break down the messengers when the job is done.
Think of the ECS as a volume dial that helps keep body systems in balance (homeostasis).
Beyond CB1/CB2 (the wider “endocannabinoidome”)
GPR55 — sometimes called a CB3-candidate; involved in pain signalling, bone health, and inflammation.
TRP channels — e.g., TRPV1, TRPA1; interact with CBD and anandamide (heat/pain, stress responses).
PPARs — nuclear receptors important for metabolism and neuroinflammation.
How it works: When a signal runs too “loud,” endocannabinoids travel backwards across the synapse and tell the presynaptic neuron to tone down. This helps balance excitatory/inhibitory signalling.
Where in the brain?
Hippocampus — memory, context, neurogenesis.
Amygdala & prefrontal cortex — fear learning, threat appraisal, anxiety, top-down control (relevant to PTSD).
Hypothalamus & pituitary — stress axis (HPA), appetite, hormones.
These circuits are often dysregulated after TBI and in PTSD; ECS signalling helps re-balance them.
How Cannabis Compounds Interact with the ECS
CBD (cannabidiol) — non-intoxicating. Supports ECS tone indirectly and also works on other targets (e.g., serotonin 5-HT1A and TRP channels) related to anxiety, sleep, and inflammation.
THC (delta-9-tetrahydrocannabinol) — intoxicating at typical doses. Partially activates CB1/CB2; at low–moderate doses may help with sleep and intrusive symptoms in some people; higher doses can impair thinking or increase anxiety in some.
Other plant components — minor cannabinoids (e.g., CBG, CBN, CBC) and terpenes (e.g., linalool, myrcene, β-caryophyllene [a CB2 agonist]) may contribute to an “entourage” effect (research ongoing).
What Current Research Suggests (Potential Benefits)
Neuroplasticity & Brain Repair
ECS signalling supports synaptic plasticity and hippocampal neurogenesis. It modulates microglia and astrocytes, damping neuroinflammatory cascades and supporting glial-neuronal cross-talk. In TBI and hypoxic injury models, ECS activity has been linked to improved recovery dynamics.
Anti-inflammatory & Immune Tuning
Activating CB2-linked pathways can reduce pro-inflammatory cytokines. CBD (and some terpenes) may contribute to calming inflammation.
Anxiety, Mood & Sleep
By influencing 5-HT1A and stress circuits, CBD shows anxiolytic and antidepressant-like effects in studies. Many report improved sleep quality and a calmer baseline.

Psychosis (CBD’s Antipsychotic Potential)
Any medication taken incorrectly (or recreationally) can trigger or worsen psychotic-like symptoms in some people. Early research and small clinical trials show CBD contains antipsychotic-like effects. Medical supervision is essential.
Seizures & Anti-Kindling
A highly purified plant-derived CBD medicine (Epidyolex) is approved by the Australian Therapeutic Goods Administration (TGA) for seizures associated with Dravet and Lennox-Gastaut syndromes. It reduces seizure frequency by stabilizing neuronal firing.
Kindling refers to a process where the brain becomes more excitable after repeated stressors or seizures, lowering the threshold for future episodes. The ECS, particularly through CB1 receptor modulation and CBD’s effects on other channels, can dampen this hyperexcitability. This is relevant not only for epilepsy but also for PTSD and TBI, where chronic stress or injury can similarly sensitize neural circuits, worsening symptoms like hypervigilance and intrusive thoughts.
Real-world Evidence & Trials
Australian registry/observational cohorts (including Special Access Scheme pathways) report use of CBD/THC for anxiety, pain, and PTSD with generally tolerable safety. Ongoing RCTs in Australia/Israel are exploring PTSD, TBI, and chronic pain.


Practical Notes (Safety & Use)
Doctor-led plan: Dosing and product choice should be guided by a clinician.
Start low, go slow: Aim for the lowest effective dose.
Day vs night goals: CBD often suits daytime; THC (if used) is often night-time.
Interactions (CYP450): CBD can inhibit CYP2C19, CYP3A4, CYP2C9, and others. This may raise levels of some medicines (e.g., clobazam, some SSRIs, warfarin). Always discuss with your prescriber and pharmacist.
Adolescent brain: Higher THC exposure during adolescence is linked with risks to neurodevelopment; be cautious and seek specialist advice.
Cardio-metabolic note: Chronic CB1 overactivation is associated with metabolic issues; clinicians may monitor weight, BP, and lipids.
Driving (Australia, 2025): Presence-based roadside testing for THC applies. NSW & QLD: presence of THC is an offence even if prescribed. VIC: presence offence still applies, but from 1 March 2025 magistrates may choose not to cancel a licence for prescribed-patient positives; fines/other penalties may still apply. Impairment driving remains illegal everywhere — always check the latest state guidance.
Who should be cautious/avoid: Pregnancy/breastfeeding; history of psychosis; unstable heart disease; uncontrolled substance use — discuss risks with your prescriber.
Quick FAQs

-
No — CBD is non-intoxicating. (THC can be intoxicating).
-
No single treatment helps everyone. ECS-based care may reduce symptoms for some people under medical supervision.
-
A specific, purified CBD medicine is TGA-approved for Dravet and Lennox-Gastaut syndromes. For other conditions like PTSD and TBI, unapproved medicinal cannabis products are accessed by doctors through the Special Access Scheme (SAS) or Authorised Prescriber pathways when conventional treatments have been ineffective.
-
Presence-based THC testing applies in NSW & QLD; in VIC, presence is still an offence but magistrates have limited discretion on licence cancellation for prescribed patients (from 1 Mar 2025); in TAS, testing if impaired occurs. Always check the latest state pages before driving.
-
No. CECD is a hypothesis about low endocannabinoid tone in some conditions. It’s a research concept, not a formal diagnosis.
-
Research suggests ECS signalling supports neuroplasticity and dampens neuroinflammation (see Section 3). Outcomes vary and should be clinician-guided.

Quick Glossary
ECS — Endocannabinoid System (your body’s self-made cannabis-like signalling).
Endocannabinoids — your own messengers (AEA/anandamide, 2-AG).
Cannabinoid receptors — CB1/CB2 (plus wider partners like TRP, GPR55, PPARs).
Entourage effect — combined plant compounds acting together.
Anti-kindling — Reducing the brain’s tendency to become more excitable over time after repeated stressors or seizures. This mechanism is key in epilepsy but is also relevant for stabilizing the fear circuits in conditions like PTSD.
CECD (Clinical Endocannabinoid Deficiency) — a working hypothesis that low endocannabinoid tone may contribute to certain conditions (e.g., migraine, fibromyalgia, IBS). It is not a formal medical diagnosis; research is ongoing.
This page is educational only and does not replace medical advice. If you’re a veteran with treatment-resistant PTSD or TBI, talk to a clinician experienced with ECS-informed care. NoMoreZombieVeterans is working to secure Department of Veterans Affairs approval and subsidy so veterans can access safer, evidence-aligned options.
References & Endnotes
Evidence snapshots behind key claims in this page. Links go to peer-reviewed journals, official regulators, or reputable medical/academic publishers. (General info only — not medical advice.)
Core overviews of the ECS / “endocannabinoidome”
Lu H-C, Mackie K. Review of the Endocannabinoid System. Biol Psychiatry Cogn Neurosci Neuroimaging (2021).https://pubmed.ncbi.nlm.nih.gov/32980261/
Iannotti F, Di Marzo V. The endocannabinoidomes: Pharmacological redundancy and promiscuity. Pharmacological Reviews (2025).
https://pharmrev.aspetjournals.org/article/S0031-6997(25)07478-2/
Beyond CB1/CB2: non-classical targets
Apweiler M, Saliba S. Modulation of neuroinflammation and oxidative stress by targeting GPR55 – new approaches in the treatment of psychiatric disorders Molecular Psychiatry (2024)
https://www.nature.com/articles/s41380-024-02614-5.pdfGray L, Tupal K. TRPV1: A Common Denominator Mediating Antinociceptive and Antiemetic Effects of Cannabinoids. International Journal of Molecular Sciences (2022)
https://www.researchgate.net/publication/363300576_TRPV1_A_Common_Denominator_Mediating_Antinociceptive_and_Antiemetic_Effects_of_Cannabinoids#Pistis M, O’Sullivan SE. The role of nuclear PPARs in cannabinoid signalling. Prog Lipid Res (2017). https://pubmed.ncbi.nlm.nih.gov/28826538/
Brain circuits relevant to PTSD/TBI/mood
Katona I, et al. Distribution of CB1 receptors in the amygdala. J Neurosci (2001).
https://pubmed.ncbi.nlm.nih.gov/11717385/Maldonado, R, et al. The endocannabinoid system in modulating fear, anxiety, and stress. Dialogues in Clinical Neuroscience (2020) https://pubmed.ncbi.nlm.nih.gov/33162766/
Neuroplasticity, neuroinflammation & glial cross-talk
Young A, The Dynamic Role of Microglia and the Endocannabinoid System in Neuroinflammation. Frontiers (2022)
https://www.frontiersin.org/journals/pharmacology/articles/10.3389/fphar.2021.806417/fullHellewell J et al. Cannabinoids in traumatic brain injury & related neuropathologies. J Neuroinflammation (2023). https://jneuroinflammation.biomedcentral.com/articles/10.1186/s12974-023-02734-9
Clinical evidence highlights
Devinsky O et al. Trial of cannabidiol for Dravet syndrome. N Engl J Med (2017).https://www.nejm.org/doi/full/10.1056/nejmoa1611618
Thiele EA et al. Cannabidiol in Lennox-Gastaut syndrome. N Engl J Med (2018).https://www.nejm.org/doi/full/10.1056/NEJMoa1714631
TGA (Australia) AusPAR — Cannabidiol (Epidyolex/Epidyolex®): indications, safety, CYP interactions.https://www.tga.gov.au/resources/auspar/auspar-cannabidiol
Leweke FM et al. Cannabidiol enhances anandamide signaling and alleviates psychotic symptoms of schizophrenia. Transl Psychiatry (2012).https://www.nature.com/articles/tp201215
McGuire P et al. Adjunctive CBD in schizophrenia (multicentre RCT). Am J Psychiatry (2018).https://pubmed.ncbi.nlm.nih.gov/29241357/
PTSD, hypervigilance & ECS dysregulation
Neumeister A et al. Elevated CB1 availability & low anandamide in PTSD (PET). Mol Psychiatry (2013).https://pubmed.ncbi.nlm.nih.gov/23670490/
Mayo LM et al. Targeting the ECS in PTSD: translational evidence. Biol Psychiatry (2021).https://pubmed.ncbi.nlm.nih.gov/34598785/
Safety nuances
Fischer A et al. Cannabis & the developing adolescent brain. Curr Treat Options Peds (2020).https://pubmed.ncbi.nlm.nih.gov/32714742/
Urbi B, et al, Effect of cannabinoids on glutamate levels in the human brain: a systematic review and meta-analysis. J of Cannabis Research (2025) https://jcannabisresearch.biomedcentral.com/articles/10.1186/s42238-025-00277-9
Kunos G et al. Peripheral CB1 blockade improves cardiometabolic risk. J Clin Invest (2010).https://pubmed.ncbi.nlm.nih.gov/20664173/
Després J-P et al. CB1 antagonism & obesity — Rimonabant RCTs. Lancet (2005/2007). https://pubmed.ncbi.nlm.nih.gov/19844251/
CBD drug–drug interactions (CYP2C19/CYP3A4):
Grayson L et al. CBD–warfarin interaction (↑INR). Epilepsy Behav Case Rep (2017).https://pubmed.ncbi.nlm.nih.gov/29387536/
Geffrey AL et al. Drug–drug interaction between clobazam and cannabidiol in children with refractory epilepsy. Epilepsia (2015). https://onlinelibrary.wiley.com/doi/abs/10.1111/epi.13060
Vaughn S, et al. The Impact of Marijuana on Antidepressant Treatment in Adolescents: Clinical and Pharmacologic Considerations. J Pers Med (2021).https://pubmed.ncbi.nlm.nih.gov/34209709/
Lifestyle & ECS tone
Siebers M, “Runner’s high” depends on endocannabinoids. Exercise-induced euphoria and anxiolysis do not depend on endogenous opioids in humans. Psychoneuroendocrinology (2021) https://www.sciencedirect.com/science/article/abs/pii/S0306453021000470
Sparling PB et al. Exercise increases circulating endocannabinoids. Br J Sports Med (2003/2004).https://escholarship.org/uc/item/426788xv
Di Marzo V, Silvestri C. Lifestyle and Metabolic Syndrome: Contribution of the Endocannabinoidome. Nutrients (2019).https://www.mdpi.com/2072-6643/11/8/1956
Plant components / “entourage”
Russo EB. Taming THC: phytocannabinoid–terpenoid synergy. Br J Pharmacol (2011).https://pubmed.ncbi.nlm.nih.gov/21749363/
Ricardi C, et al. β-caryophyllenea Cannabinoid Receptor Type 2 Selective Agonist, in Emotional and Cognitive Disorders. Int J Mol Sci (2024).https://pmc.ncbi.nlm.nih.gov/articles/PMC10970213/
CECD (working hypothesis)
Russo EB. Clinical endocannabinoid deficiency reconsidered. Cannabis Cannabinoid Res (2016).https://pubmed.ncbi.nlm.nih.gov/28861491/
Russo EB. Clinical Endocannabinoid Deficiency (overview & early proposal). Neuroendocrinology Letters (2004).https://www.nel.edu/userfiles/articlesnew/NEL251204R02.pdf
Seizure science: kindling background
Morimoto K. Kindling and status epilepticus models of epilepsy: rewiring the brain. Prog Neurobiol (2005).https://pubmed.ncbi.nlm.nih.gov/15193778/
Singh T, et al. PTZ kindling model for epileptogenesis (review). Metab Brain Dis (2021).https://pubmed.ncbi.nlm.nih.gov/34427842/
Australian driving laws (THC presence offences; reforms ongoing)
NSW Medicinal Cannabis — Medicinal cannabis & driving (presence of THC is an offence).https://www.medicinalcannabis.nsw.gov.au/patients/driving
NSW Drug Summit Backgrounder (Nov 2024) — overview of NSW framework & driving laws. https://www.health.nsw.gov.au/aod/summit/Documents/2024-nsw-drug-summit-report.pdf
Victoria (Transport) — Medicinal cannabis & driving (presence-based law).https://www.vicroads.vic.gov.au/safety-and-road-rules/driver-safety/drugs-and-alcohol/medicinal-cannabis-and-driving/
Victoria (Transport) — Drug-driving penalties (from 1 Mar 2025: magistrate discretion on licence cancellation for prescribed patients; presence offence still applies).https://transport.vic.gov.au/road-and-active-transport/road-rules-and-safety/alcohol-drugs-and-driving/medicinal-cannabis-and-driving
Queensland (TMR) — presence-based testing & offences.https://www.qld.gov.au/transport/safety/road-safety/drink-driving/drugs
Trials & registries (PTSD/TBI & pain)
Blessing EM (NYU). CBD for PTSD (with/without TBI) RCT. https://clinicaltrials.gov/study/NCT04550377
Australian clinical trials / ANZCTR portal (search: “cannabidiol PTSD”, “traumatic brain injury”).https://onlinelibrary.wiley.com/doi/10.1111/jsr.13793
